Non-Surgical Prostate Cancer Treatment
Hormone Therapy
What is prostate cancer hormone therapy?
Hormone therapy, or androgen deprivation therapy (ADT), is used to suppress a man’s testosterone level in hopes of starving the prostate cancer tumor. It is suitable for cases of advanced prostate cancer and the goal is to shrink the tumor or cause it to grow more slowly. Androgen deprivation therapy is not a prostate cancer cure.
Is hormone therapy right for me?
Since hormone therapy does not remove the prostate or eliminate prostate cancer, it does not provide the same level of cancer-free assurance as robotic prostate removal. Hormone therapy may be best suited for men of advanced age, those who are not surgical candidates, or for those whose cancer has returned.
What are the side effects of prostate cancer hormone therapy?
Bone weakening and bone loss are the primary concerns associated with hormone therapy. Cancer Treatment-Induced Bone Loss (CTIBL) related to ADT is widely studied and proven. A 10-year study published in 2013 demonstrated that ¼ of hip fracture patients had previously been treated with ADT for low-risk prostate cancer.
Kidney damage is another concern resulting from hormone therapy. A separate 2013 study found a significantly increased risk of acute kidney injury (AKI), among hormone therapy patients with advanced, non-metastatic prostate cancer.
A decrease in testosterone leads to a loss of muscle mass and an increase in fat, that can have serious side effects in men, including the development of heart disease. Applying prevention measures for ADT side-effects can help reduce this outcome.
Other potential side effects of hormone therapy include:
- Impotence and/or loss of libido
- Testicle and penis shrinking
- Hot flashes and breast tenderness
- Osteoporosis and anemia
- Fatigue and depression
Prostate Cancer Radiation
How is radiation used to treat prostate cancer?
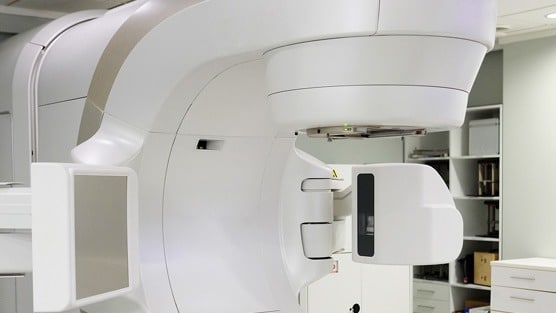
Using external beam radiation therapy (EBRT) or brachytherapy seed implants, radiation can be used to target prostate cancer tumors.
Is radiation therapy right for me?
Like hormone therapy, radiation therapy does not remove the prostate gland or the prostate cancer. After treatment, PSA levels can continue to fluctuate and require frequent monitoring. EBRT can be an effective second line of defense against prostate cancer. If cancer should return after surgery, radiation can be used for long-term disease control with positive survival rates. What if I have radiation before surgery?
What if I have radiation before surgery?
In most cases, robotic prostate surgery cannot be performed after radiation treatment. This is a very important treatment consideration. Radiation alters the prostate tissue in such a way that surgery is typically not an option for disease recurrence. For this reason, many men reserve radiation treatment until after surgery. Even then, follow-up treatment after robotic surgery is typically not needed.
What are the side effects of radiation treatment?
After radiation treatment for prostate cancer men may experience side effects such as:
- Difficulty urinating and emptying the bladder
- Burning sensation during urination
- Scrotal, rectal, and perineal discomfort
- Research also indicates that radiation for prostate cancer could increase a man’s risk of developing bladder cancer and rectal cancer.
CyberKnife®
What is CyberKnife® for prostate cancer?
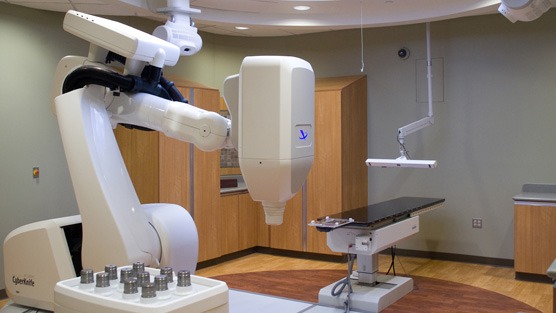
CyberKnife Robotic Radiosurgery is not surgery, but simply a brand name for high-dose radiation. The treatment is conducted over a series of 1-5 sessions to administer Stereotactic Body Radiation Therapy (SBRT).
Is CyberKnife right for me?
CyberKnife is FDA approved, but because the procedure is so new there is very little data regarding its effectiveness in treating prostate cancer. The makers of CyberKnife recommend it for low-risk prostate cancer. However, since CyberKnife is radiation therapy it may preclude the ability to have robotic prostate surgery later.
What CyberKnife side effects should I be concerned about?
Like radiation, CyberKnife can cause problems with urination and irritation of the anus and rectum. Long-term, CyberKnife patients can experience sexual impotence and erectile dysfunction (ED) for up to 2 years. Bowel function can also be impacted, and risk of bladder cancer and rectal cancer can increase by as much as 5%.
What else should I know about CyberKnife?
During CyberKnife treatment, radiation is administered to the prostate based on imaging gathered before and during the procedure. Unlike the first-hand analysis afforded by surgery, CyberKnife is essentially a “best guess” treatment about where the cancer is located and how extensive it may be. There is no post-surgery tumor analysis, nor a zero PSA.
HIFU
What is HIFU?
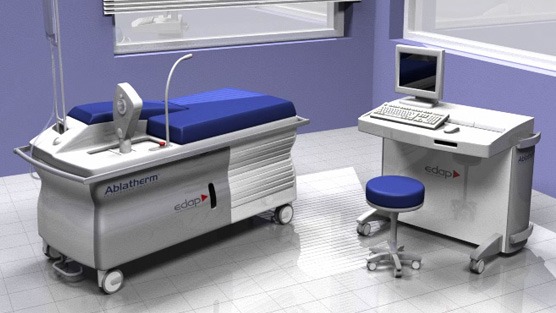
HIFU (High Intensity Focused Ultrasound) is an experimental prostate cancer treatment that is not FDA approved. Using radiation-free sound waves via rectal probe, HIFU is used to cover the prostate with High Intensity Focused Ultrasound energy. The diseased tissue is heated and destroyed, to later be expelled naturally by the body.
Is HIFU right for me?
HIFU cannot be performed in the United States; it is not FDA approved; and it is not covered by insurance. As a new treatment modality, there is very limited data about the effectiveness of HIFU for prostate cancer. Like radiation and hormone therapy, HIFU is designed to treat prostate cancer, but not remove it. Each treatment of this kind requires men to adhere to a rigorous post-treatment regimen to monitor the possibility of prostate cancer recurrence.
What are the side effects of HIFU?
Some studies indicate that as many as 70% of men who undergo HIFU are left permanently impotent. Other reported side effects include:
- ED and ejaculation problems, including internal ejaculation
- Urinary frequency, burning, and incontinence
- Injury to the rectal wall or rectal incontinence
- Prostate infection
- Long-term catheter use for up to a month
Active Surveillance/Watchful Waiting
Do I have to treat my prostate cancer?

All healthcare decisions are personal and should be made after gathering all of the facts, exploring treatment options, and discussing lifestyle goals with your loved ones. Based on age, overall health, and personal beliefs, some men choose not to treat their prostate cancer.
What are Active Surveillance and Watchful Waiting for prostate cancer?
Both terms are used to define patients who choose not to treat their prostate cancer upon diagnosis. These men are encouraged to follow very aggressive testing regimens to watch for changes in their disease. Prostate cancer can spread slowly or very quickly and without warning. As such, the decision not to treat prostate cancer may weigh heavily on men over the long-term.
How risky is it to postpone prostate cancer treatment?
Beyond the obvious risk of disease advancement, the decision to delay prostate cancer treatment can lead to increased anxiety and depression among men. Some patients report feeling like they have a ticking time bomb in their bodies, wondering if the disease is spreading or not.
Working with a prostate cancer expert like Dr. Samadi can help you assess the likelihood of disease spread based on your diagnosis and individual risk factors.
Other men choose active surveillance based on the potential side effects of treatment or other concurrent health issues. Since older men are more likely to develop prostate cancer, it is possible for a separate medical condition to take precedence over prostate cancer treatment.
Make sure to read about the other treatment options:
Bibliography
- Hormone therapy for prostate cancer, American Cancer Society, Web.
- HIFU Prostate Cancer Treatment, PubMed Abstract, Web, Sept 2018.
- Cyberknife Radioablation of Prostate Cancer, PubMed Abstract, Web, 2017.
- Radiation Therapy for Prostate Cancer, PubMed Abstract, Web, MAr-Apr 2019.

